The field of sleep medicine suffers a blind spot by neglecting the pioneering work of the ultra-brilliant neurologist, sleep physician and researcher, Dr. Christian Guilleminault (1939-2019), who discovered the upper airway resistance syndrome (UARS) in children in the early 1980s and in adults in the early 1990s. He was my mentor in the spring of 1993, not long after this landmark work.
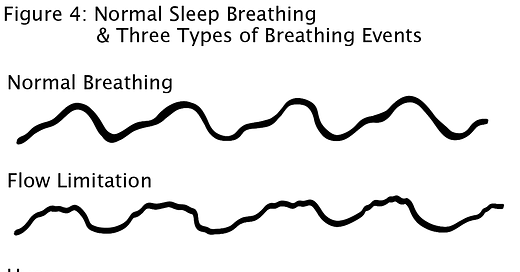
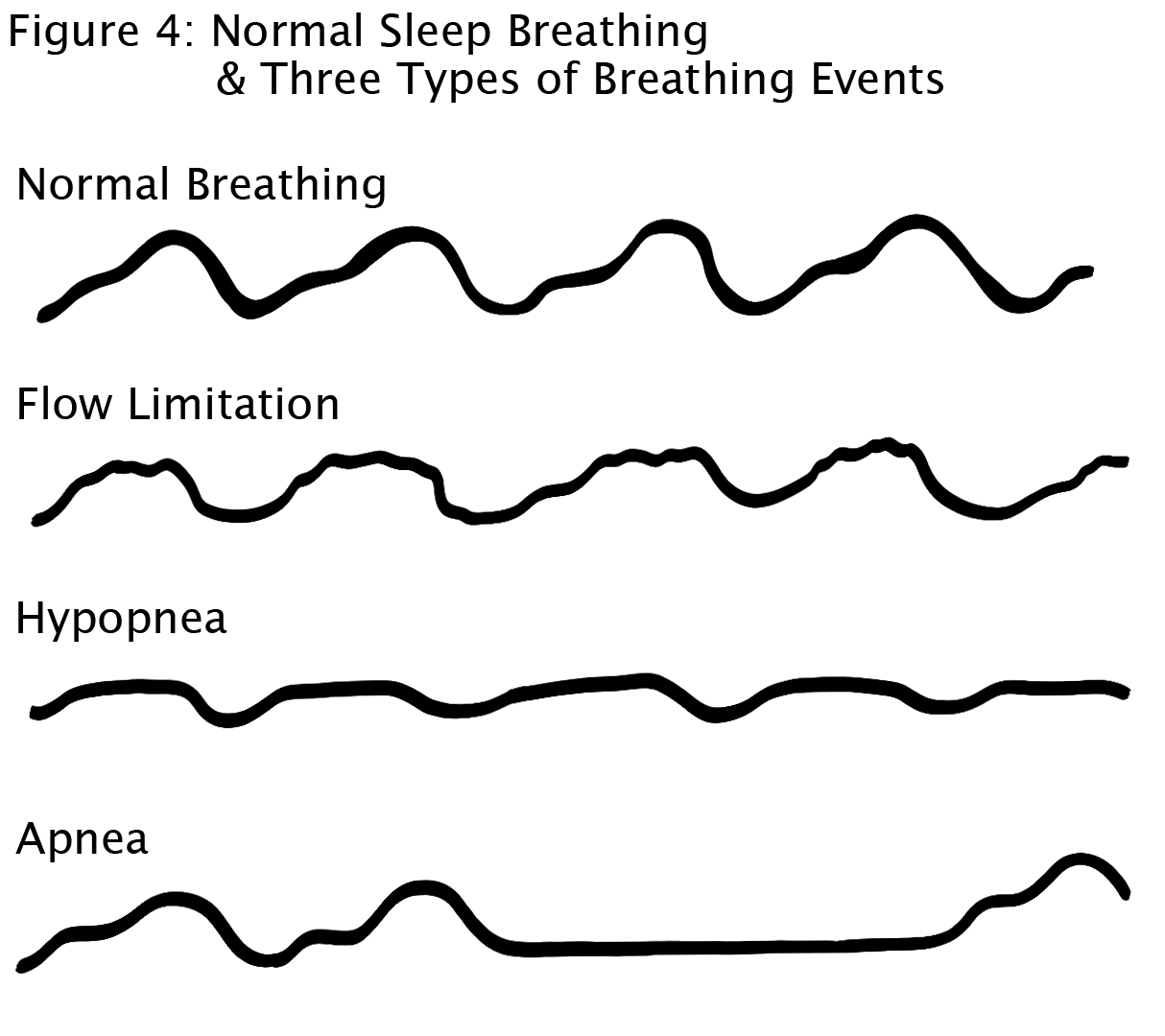
UARS is the source of the 3rd breathing event and must be distinguished from the two more commonly discussed events: apneas and hypopneas. You lose nearly 100% of all breath volume of air during apneas, ~50% loss during hypopneas, and about 25% (sometimes even smaller) loss during UARS events. In the diagram below (that will appear in my forthcoming book) you can see the differences comparing normal breathing to sleep breathing events. Notice the rounded shapes in the normal breathing compared to increasing flattening changes on the top half of the curves for flow limitation and more so with the hypopnea. With apnea, you lose the entire breath.
UARS is a general category, whereas a UARS specific breathing event is named respiratory effort-related arousal (RERA), although most sleep professionals prefer flow limitation or flow limitation events. The term RERA shows up (if it shows up at all) on your sleep study, so it’s a good idea to know both these terms describing the 3rd breathing event.
What’s the big deal about this 3rd breathing event? Very simply, if your sleep breathing disorder comprises only these events, meaning you suffer from the diagnosis of UARS and no apneas or hypopneas, then this condition still causes or is linked to nearly all the same problems as someone who suffers from the more commonly known obstructive sleep apnea (OSA). For example, UARS causes insomnia, nocturia (trips to the bathroom at night), daytime fatigue and sleepiness, and…drum roll please….UARS causes high blood pressure.
You would think with these obvious health connections sleep professionals would scrutinize your sleep studies to clarify and confirm whether you are suffering from flow limitation events (aka RERAs). Unfortunately, most sleep centers pay scant attention to this 3rd event, due to three barriers.
First, many sleep professionals are ignorant of the condition. Because they know nothing about UARS, they would not think to look for flow limitations on your sleep studies.
Second, they may know of UARS but exhibit no respect whatsoever for the condition. How could sleep professionals ignore a condition that causes insomnia, nocturia, tiredness, sleepiness and hypertension? I discussed some of these points in an earlier book.
Third, they may be interested in UARS, but they report difficulty trying to score this 3rd type of event on an airflow tracing signal, because in a nutshell it’s easier to measure a breathing problem when you are losing 50 to 100% of your air volume compared to only 25%.
For all these reasons and many more, only a small minority of sleep professionals closely scrutinize and accurately measure the problem of UARS. And, please note, even when your diagnosis is OSA, chances are astronomically high you also suffer some proportion of UARS as well. As such, this minority of sleep doctors are usually the ones who know the necessity to aggressively treat your flow limitation events, because it certainly makes a lot of sense to treat a condition that will improve your insomnia, nocturia, tiredness, sleepiness and hypertension.
The point being, it is in your best interest to ask your sleep doctors how they approach the problem of UARS, including how they specifically score the RERAs on your sleep studies and how they aggressively treat your flow limitations with a PAP device or other therapy.